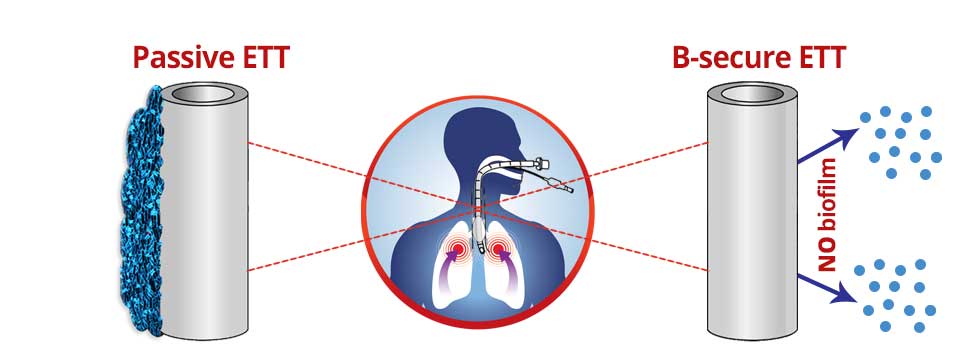
Ventilator-associated pneumonia (VAP) is defined as pneumonia that occurs 48-72 hours or thereafter following endotracheal intubation, contributes to approximately half of all cases of hospital-acquired pneumonia. VAP is estimated to occur in approximately 20% of all mechanically ventilated patients, with the highest risk being early in the course of hospitalization. It is the second most common nosocomial infection in the intensive care unit (ICU) and the most common in mechanically ventilated patients. ventilator-associated pneumonia (VAP) occurs at most, due to intubation of endotracheal tubes (ETTs) or tracheostomy tube, and is associated with increased hospital length of stay, mortality, infections due to multidrug-resistant bacteria, and an attributable hospital cost of approximately $10,000 to $25,000. Therefore, preventive measures that could impact the incidence of VAP in the intensive care units (ICU) setting must be considered a priority, because they could improve the safety of patients in the ICU.